P222 Chronic pain is common in Paediatric Inflammatory Bowel Disease and impacts quality of life
Mardare, R.(1)*;Eskell, L.(1);Machta, J.(1);Fell, J.M.E.(1);Thangarajah, D.(1);
(1)Chelsea and Westminster Hospital, Paediatric Gastroenterology, London, United Kingdom;
Background
Prevalence of chronic pain (CP) is reported as 38% in adult inflammatory bowel disease (IBD), with a significant impact on quality of life, functional and social outcomes 1,2,3. Prevalence and attributes of chronic pain are unknown in paediatric IBD. Aim: evaluate the prevalence, disease related factors, and impact on quality of life (QOL) of CP.
Methods
Prospective, cross-sectional single centre study included 41 children, (8 -18 years), of a predominantly CD cohort 29/41, (70%). Patients and their parents completed validated age-appropriate pain questionnaires4 and IMPACT III QOL questionnaire for IBD5. CP was defined mild and moderate to severe, as per von Korff scale6. Disease specific parameters were recorded. CP and NP medians were compared using Mann-Whitney tests and proportions using Chi squared test (p<0.05).
Results
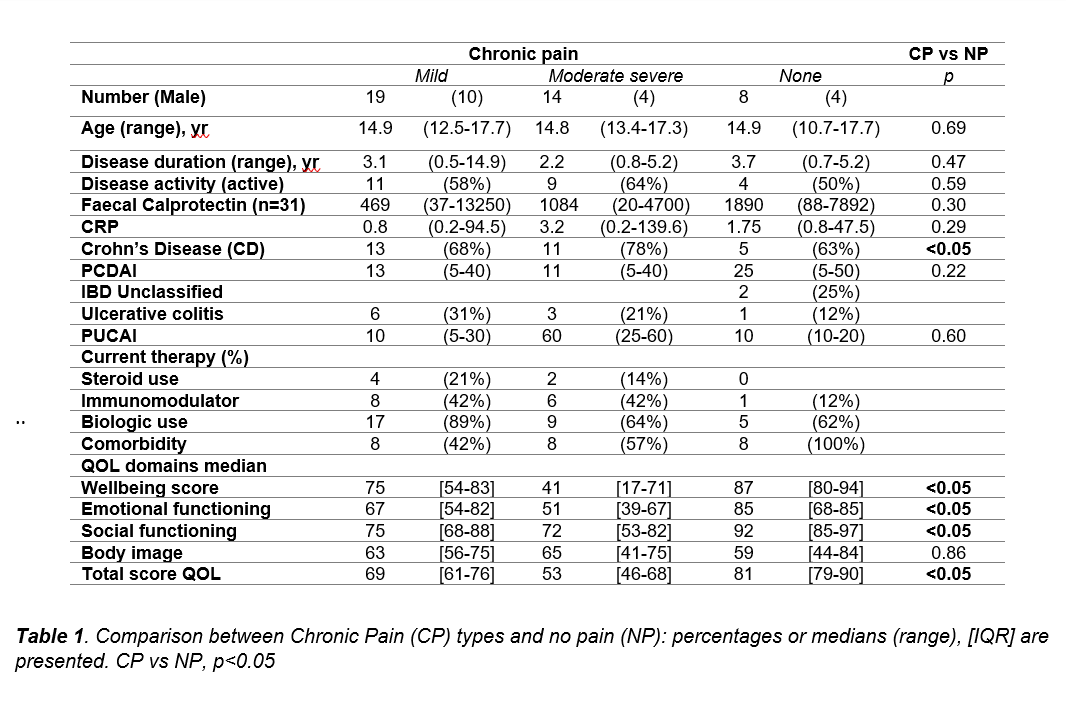
CP was prevalent in 33/41 (80%) patients. Abdominal CP was common in 30/33 (90%), joint pain was present in 2/33, (6%) and headache in 1/33, (3%). CP subjects were adolescents with extensive and established disease, predominantly on biologics 26/33 (79%). Analgesia use was low 15/33 (45%), and there was no opiate use. There was no difference in Disease activity CP vs NP, defined by PCDAI, PUCAI, CRP and Faecal calprotectin. QOL life score was significantly lower in CP, there was no difference in body image QOL domain score in CP vs NP. Comorbidity was common 16/33 (48%) in the CP cohort, 5/16 (31%) had diagnoses that maybe associated with comorbid pain.
We have shown that anaemia and sleep disturbance may be a signal associated with CP (Fig 1).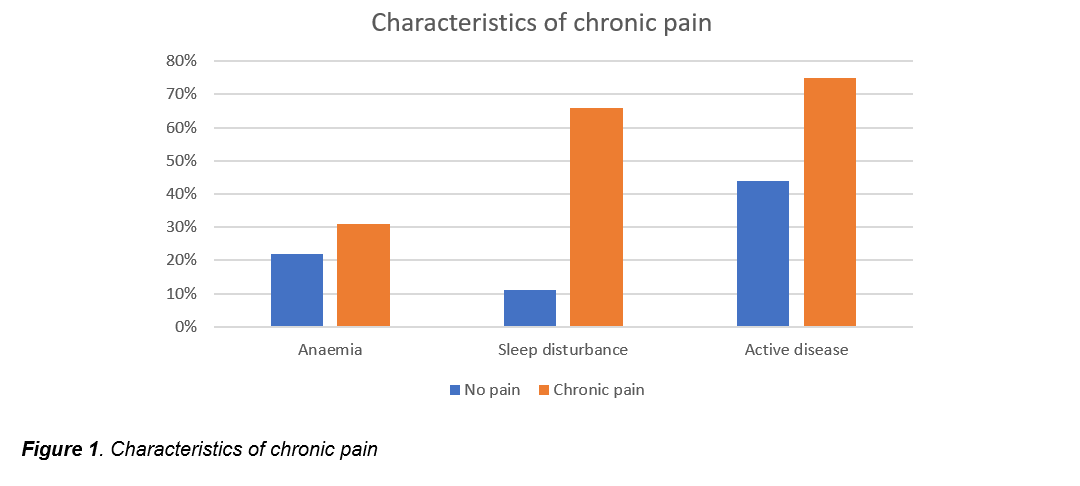
Conclusion
CP is common in paediatric IBD, more common than previous adult studies. Unlike historic adult IBD cohorts, it is not associated with disease activity or related biomarkers. It is unknown whether functional pain co-exists in our cohort. CP significantly impacts emotional, wellbeing and social functioning in children with IBD. This is the first study to report on CP in children with IBD, strategies should target psychosocial intervention. Further studies are needed to evaluate potential effects of socioeconomic status, physical activity, anaemia and prevalence of functional pain in children with IBD. We recommend screening for CP in children with IBD as it is common.


