P224 Diagnostic delay in inflammatory bowel disease is not associated with difficult access to healthcare facilities: a clinical study on incidental cases
Cantoro, L.(1)*;Monterubbianesi, R.(1);Camastra, C.(1);Falasco, G.(1);Pantanella, P.(1);Cosintino, R.(1);Faggiani, R.(1);Fiorino, G.(1,2);
(1)Azienda Ospedaliera San Camillo-Forlanini, IBD Unit- Department of Gastroenterology and Digestive Endoscopy, Rome, Italy;(2)Vita e Salute University, Gastroenterology and Digestive Endoscopy, Milan, Italy;
Background
Diagnostic delay is a challenge in inflammatory bowel disease (IBD), more in Crohn’s disease (CD) than in ulcerative colitis (UC). Whether difficult access to healthcare facilities may be a cause of diagnostic delay is debated. Restrictions due to SARS-COV2 pandemic have impacted on the prompt access to hospitals and clinics during 2020. We aimed to investigate if those limitations impacted on diagnosis, presence of IBD-related complications, and the number of hospitalization and surgeries by the first 12 months after diagnosis.
Methods
We retrospectively analysed all consecutive patients who had access to our tertiary referral centre in Rome, Italy in the period between January 1st, 2019 and December 31st, 2021. We split all patients in three study groups: those who had diagnosis of IBD in 2019 (normal setting, control group), 2020 (severe restrictions for access to our clinic), and 2021 (intermediate restrictions). Delay from symptoms to diagnosis, presence of IBD-related complications at diagnosis, need for hospitalization and/or surgery at diagnosis, and hospitalization and surgery rates in the first 12 months since diagnosis were collected and analysed. Statistically significant differences were set as per p value <0.05.
Results
Overall, 6,125 patients accessed to our department in 2019, 4,594 in 2020, and 6,063 in 2021. In the entire period, 89 patients were diagnosed with IBD (17 CD and 14 UC in 2019, 12 and 10 in 2020, and 17 and 19 in 2021). Baseline characteristics are listed in Table 1. Median delay between symptoms and diagnosis did not statistically differ among the 3 groups (7 months in 2020, and 2 months in 2021, compared to controls, p=0.07 and p=0.24 respectively), and among CD and UC patients (p=0.30). No differences were found in hospitalisation at diagnosis (p=0.90 for 2020, and p=0.66 for 2021 compared to controls), and in the rates of IBD-related hospitalization and surgery in the following 12 months since diagnosis (p=0.41 for 2020, 0.81 for 2021 compared to controls). No significant associations were found between CD and UC patients, and no significant association was found between sex, age, type of disease, and localisation of the disease at diagnosis and 12-month outcomes. 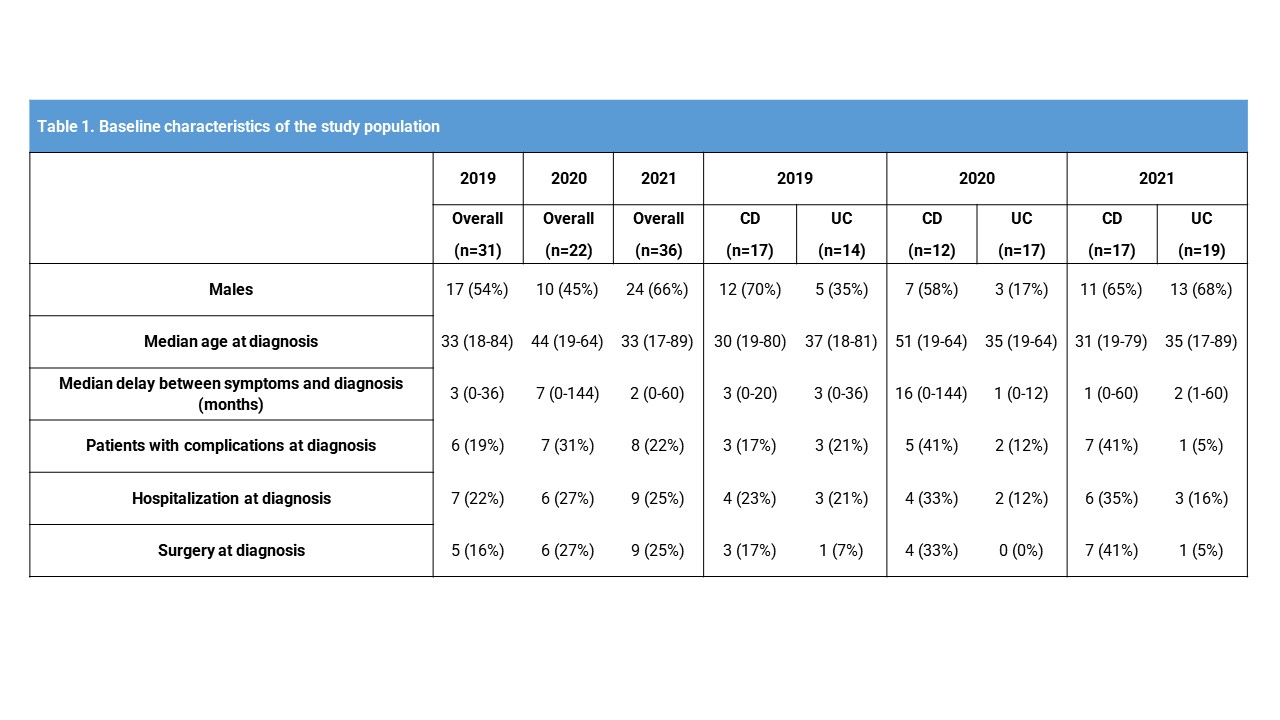
Conclusion
Although on a small population, difficulties in accessing to hospital did not impact on diagnostic delay and further disease course in IBD patients. Further investigation on factors associated with diagnostic delay is needed.


