P238 The ‘Malnutrition Universal Screening Tool’ (MUST) is less effective than an IBD specific Malnutrition Inflammation Risk Tool (MIRT) in identifying malnutrition risk with hospital admissions and surgical complication
xia, Q.(1);Mujiri, S.(2)*;Syme, G.(2);Mehta, S.(1);
(1)Barts Health NHS Trust, Gastroenterology, London, United Kingdom;(2)Barts Health NHS Trust, Nutrition and Dietetics, london, United Kingdom;
Background
IBD is associated with altered body composition and micronutrient deficiencies. None of the existing validated nutritional screening tools can correctly identify nutritional deficiencies in IBD. MUST is a widely used malnutrition screening tool in the UK. However, it failed to present relevance to clinical outcomes, while a newly developed IBD-specific tool, MIRT, showed significant correlations in CD patients.
Methods
Two single-centred retrospective projects were conducted in IBD tertiary centre at Royal London Hospital. Study A focused on IBD inpatients during the year 2021 with hospital stays ≥7 days 69 patients (43 males and 26 females), while study B examined 49 who underwent IBD-related surgery admitted between October 2019 and March 2022. They share the same defining criteria in MUST and MIRT. Hospital length of stay (LoS) and Clavien-dindo grade (CDG) were used to assess the clinical outcomes in surgical patients (study B).
Results
Study A: There were significant differences between MIRT and MUST in identifying the risk of malnutrition (Chi-square statistics =1.817, df =1, p =0.178). Fisher’s exact test P=0.239. and accepted alternative hypothesis. MIRT identified a significantly higher proportion of patients with the risk of malnutrition in comparison to MUST (strengths of relationship k=0.165 [95% CI] p =0.178). An independent sample t-test was undertaken to determine the association between malnutrition -MUST ≥2 and LoS. It was found that there was no difference between the means of the two groups and the LoS. t (32) =-0.002 p=0.998 P>0.05. Similarities have been found with MIRT≥3 score and association with LoS t (67) = -0.158 p=0.875 p>0.05Study B: The MUST did not significantly correlate with CDG or LoS (ρ =0.145, P =0.322; ρ = 0.033, P =0.823); however, the MIRT score did (ρ = 0.339, P =0.017; ρ =0.399, P = 0.005). The MIRT is thus a better NST than MUST in correlating with surgical outcomes within the IBD patient population. A higher MIRT score of ≥3 was significantly associated with both CDG (P =0.009) and hospital LoS (P =0.003), while a higher MIRT score ≥2 was not significantly associated with either (P =0.272; P =0.095) shown in Table 1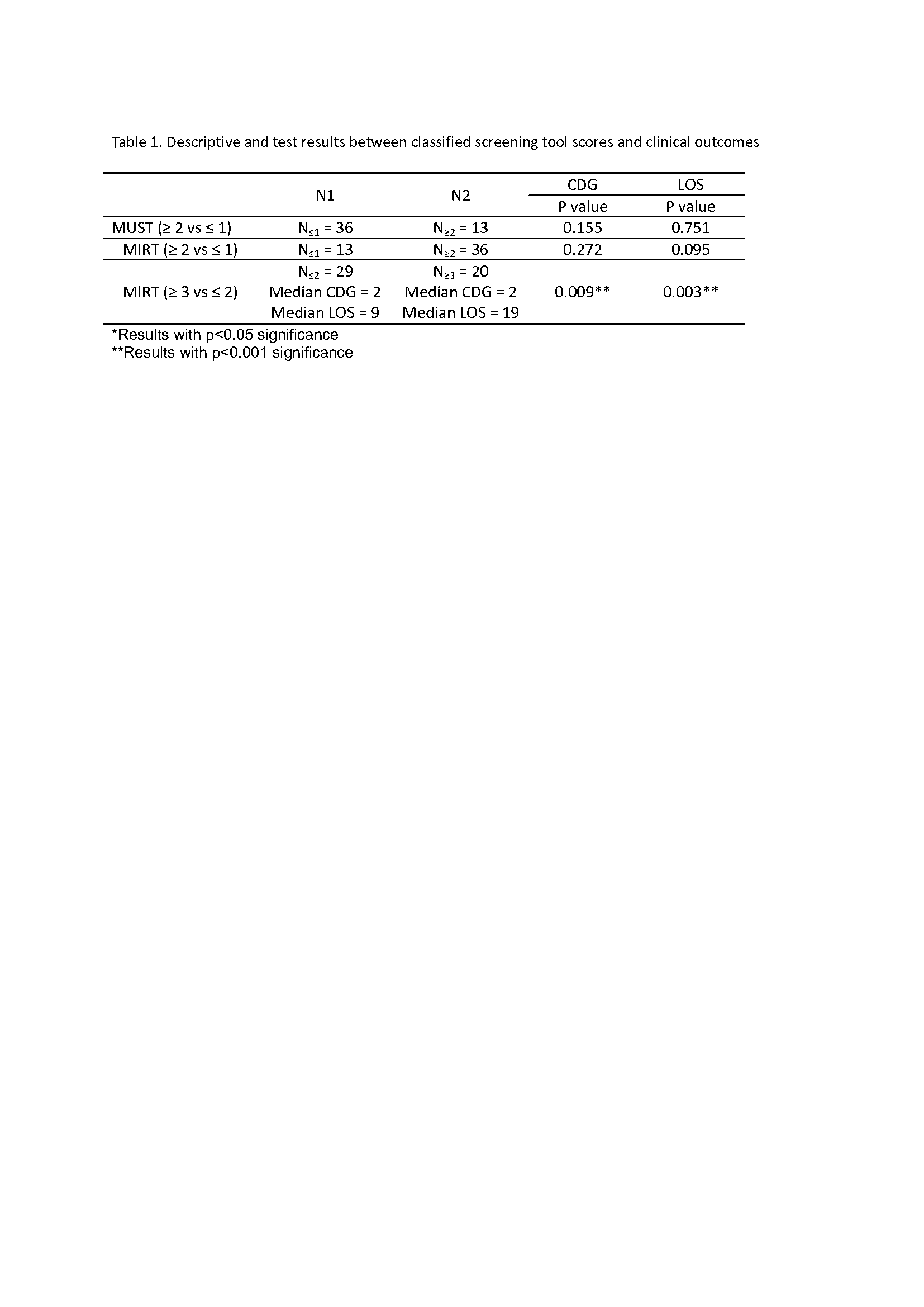 .
.
Conclusion
MIRT identifies a higher proportion of malnutrition in IBD patients 1 week from admission, but there is no direct correlation with complications and LoS. However, the opposite is the case in surgical patients where MIRT is a better pre-indicator for longer stays and complications. Having a disease-specific tool that correctly identifies the risk of malnutrition and predicts disease clinical outcomes in the IBD inpatient setting will improve the quality of healthcare and also will reduce healthcare costs. Further studies are needed ideally prospectively.


