P290 Development of an artificial intelligence model using stool pictures for predicting endoscopic mucosal inflammation in patients with Ulcerative Colitis; KASID multicenter study
Kim, E.S.(1)*;Lee, J.W.(1);Kim, S.K.(1);Lee, H.S.(1);Lee, Y.J.(2);Kim, J.(2);Kim, K.O.(3);Jang, B.I.(3);Kim, E.Y.(4);Jung, Y.J.(1);Park, S.K.(5);Park, D.I.(5);Woo, D.(6);Jeong, S.(6);
(1)Kyungpook National University Hospital, Internal Medicine, Daegu, Korea- Republic Of;(2)Keimyung University School of Medicine, Internal Medicine, Daegu, Korea- Republic Of;(3)Yeungnam University College of Medicine, Internal Medicine, Daegu, Korea- Republic Of;(4)Daegu Catholic University School of Medicine, Internal Medicine, Daegu, Korea- Republic Of;(5)Kangbuk Samsung Hospital- Sungkyunkwan University School of Medicine, Internal Medicine, Seoul, Korea- Republic Of;(6)Research Center for Artificial Intelligence in Medicine- Kyungpook National University Hospital, Medical Informatics, Daegu, Korea- Republic Of; IBD Research Group of KASID
Background
Disease monitoring through objective measures including fecal calprotectin and endoscopy is crucial for the management of ulcerative colitis (UC). The role of stool pictures taken by smart phones in the disease monitoring of UC is not known. We aimed to develop artificial intelligence (AI) model using stool pictures for predicting endoscopic mucosal inflammation in patients with UC.
Methods
This was a prospective multicenter study conducted in 6 tertiary referral hospitals. Patients scheduled to undergo endoscopy for monitoring of mucosal inflammation were included in the study. They were asked to send their stool photos taken at the toilet using smartphones within ± 5 days from the day of endoscopy. Endoscopic activity was assessed with Ulcerative Colitis Endoscopic Index of Severity (UCEIS). 80% and 20% of total data were randomly selected as training and validation set, respectively and this process repeated 4 times on different iterations for cross-validation. Accuracy of AI model for predicting endoscopic healing was compared with that of fecal calprotectin (Fcal).
Results
A total of 2463 stool pictures from 293 patients with UC were collected (mean age, year, 44±15.2; female, 108 (36.9%)). Endoscopic healing was found in 165 patients (56.3%). In validation set, the mean area under the receiver operating characteristic (AUROC) for predicting endoscopic activity using AI model was 0.78±0.02 (p=0.001) which was not statistically different from the AUROC of Fcal (0.81±0.08, p=0.01; AI model vs. Fcal p>0.05). When we excluded rectal sparing cases (20, 6.8%), the mean AUROC of AI model increased to 0.85±0.05 (p=0.0007). Accuracy, sensitivity and specificity of AI model for predicting endoscopic activity in all patients and without rectal sparing cases were 0.739, 0.643, and 0.826, and 0.798, 0.711, and 0.872, respectively. 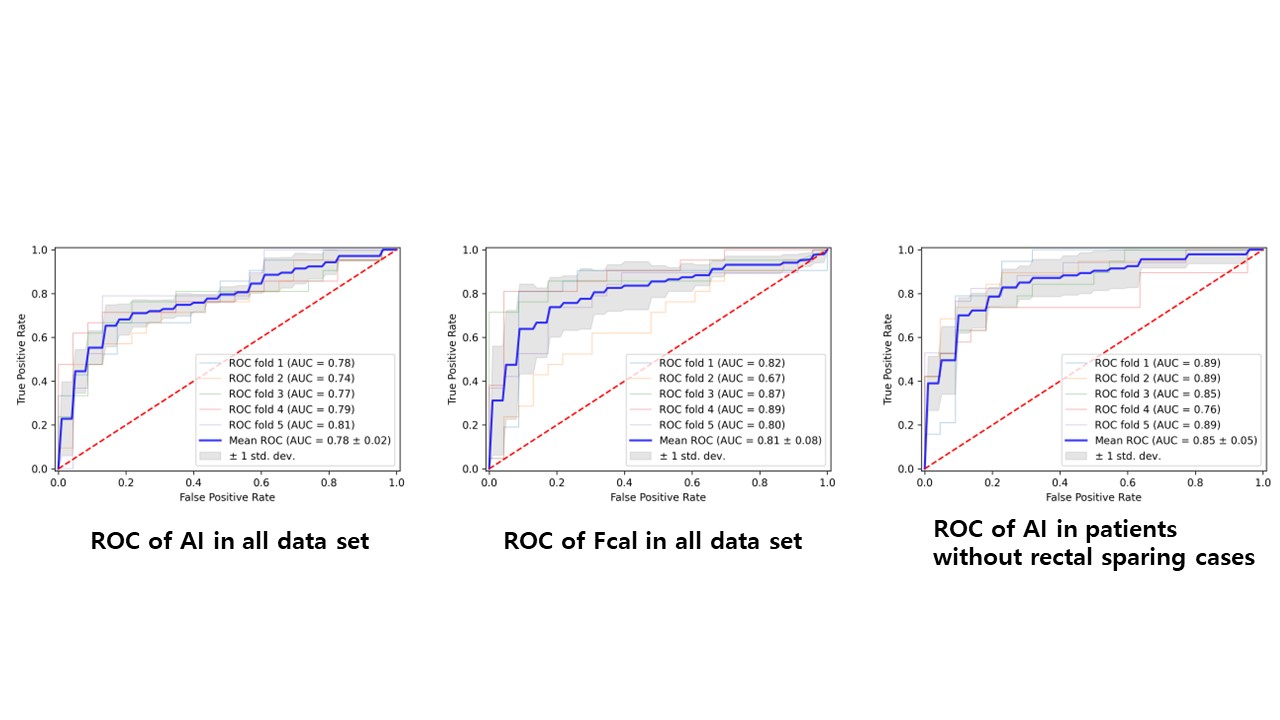
Conclusion
Stool photos of UC patients with deep learning technology demonstrated similar accuracy to Fcal in speculating endoscopic activity with better accuracy in patients without rectal sparing. The potential of simple stool pictures as a possible monitoring tool for UC activity is hopefully presented in this study.


