P292 Complications in elderly-onset Inflammatory Bowel Diseases – A population-based study from the epidemiological database of the Israeli IBD Research Nucleus (Epi-IIRN)
Ben Hur, D.(1)*;Lebedenko, B.(2);Issaschar, G.(3);Moshe, R.(3);Lujan, R.(4);Focht, G.(4);Loewenberg Weisband, Y.(5);Kariv, R.(6);Ledderman, N.(7);Matz, E.(8);Dotan, I.(9);Turner, D.(4);Pinto, G.(3);Waterman , M.(1);
(1)Rambam Health Care Campus, Department of Gastroenterology, Haifa, Israel;(2)Rambam Health Care Campus, Clinical Epidemiology Institute, Haifa, Israel;(3)Azrieli College of Engineering, Department of Industrial Engineering and Management, Jerusalem, Israel;(4)Shaare Zedek Medical Center- The Hebrew University of Jerusalem, The Juliet Keidan Institute of Pediatric Gastroenterology and Nutrition, Jerusalem, Israel;(5)Clalit Health Services, Clalit Research Institute- Innovation Division, Tel Aviv, Israel;(6)Maccabi Health Services, Maccabi Health Services, Tel Aviv, Israel;(7)Meuhedet Health Services, Meuhedet Health Services, Tel Aviv, Israel;(8)Leumit Health Services, Leumit Health Services, Tel Aviv, Israel;(9)Rabin Medical Center, Division of Gastroenterology-, Petah Tikva, Israel;
Background
The population of elderly-onset (diagnosis >=65 years old) inflammatory bowel disease (IBD) is growing worldwide. Management of this population poses challenges, given the overall increased morbidity at the elderly age. Data related to complications in this population are limited. We performed a population-based study of elderly IBD patients to characterize complications compared with non -IBD matched individuals.
Methods
As part of the validated epidemiological cohort of the Israeli IBD Research Nucleus (epi-IIRN), we included all elderly-onset IBD patients (age at diagnosis >65 years) from the four Israeli health funds diagnosed from 1.1.2005 until 30.06.2020, covering 98% of the Israeli population. Each IBD case was matched at diagnosis to 3 non-IBD individuals by year of birth, sex, geographic district, and health fund. Comparison of incidence of pneumonia, osteoporotic fractures, bacteremia/septicemia and venous thromboembolism events were made. Time to complication was compared using the Kaplan-Meier survival analysis, stratified by IBD subtype, sex and any exposure of >3 months to immunosuppressive IBD medications. Cox proportional hazard models were sought to explore complications risk adjusted by comorbidities (chronic obstructive pulmonary disease, ischemic heart disease and other diseases).
Results
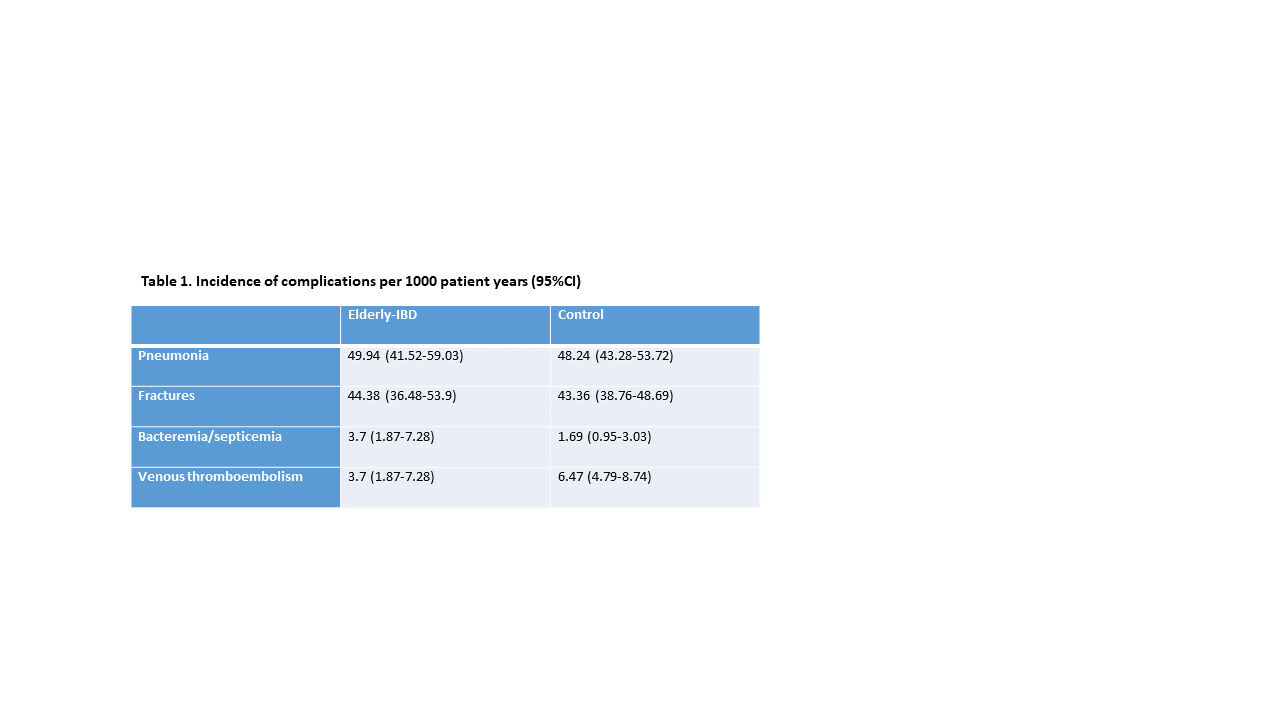
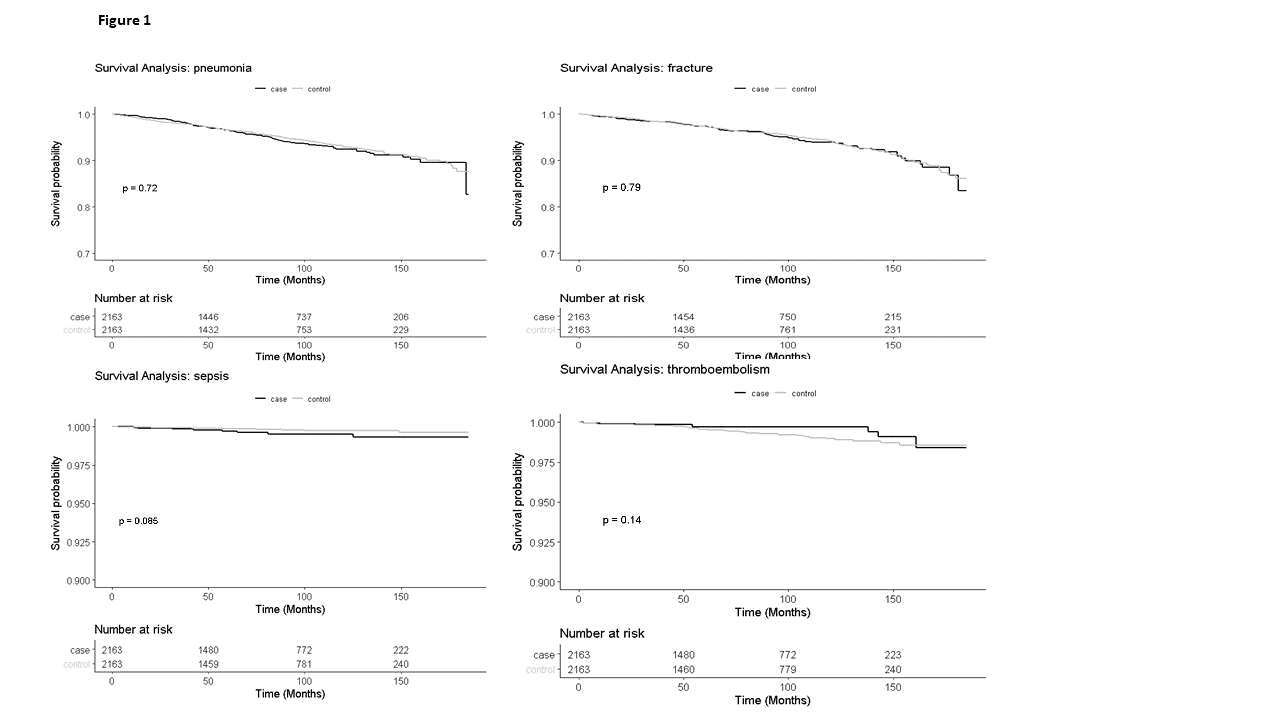
A total of 2,163 elderly-onset IBD patients were identified (46% males; 48% with Crohn’s disease, median (IQR) age at inclusion 71 [68, 76] years, exposure to >3 months of systemic CS 25%, thiopurines 10%, methotrexate 3.3%, anti-TNF 10.2%, Vedolizumab 5.7%, Ustekinumab 1.7%) and compared to 6,489 matched non-IBD controls. Median (IQR) follow-up time was 74 (40, 118) months. Incidence rates of pneumonia, fractures, bacteremia and venous thromboembolism are shown in table 1. On univariate analysis event-free survival analyses were similar in IBD and controls in pneumonia (p=0.72), osteoporotic fractures (p=0.79), bacteremia (p=0.085) and venous thromboembolism (p=0.14) Figure 1. Survival analysis remained similar when stratified by sex, IBD subtype and drug exposure. Using the comorbidity adjusted Cox model, the overall HR of pneumonia was 1.04 (95% CI 0.835-1.294), for osteoporotic fractures was 1.026 (95% CI 0.815-1.293); of bacteremia 2.161 (95% CI 0.865-5.397) and of venous thromboembolism 0.579 (95% CI 0.272-1.23).
Conclusion
In this population-based nation-wide study elderly onset IBD was not associated with increased risk of pneumonia, bacteremia, venous thromboembolism, and osteoporotic fractures compared with matched non-IBD elderly individuals. Studies in other populations are still needed to assess complications risk in diverse populations.